The liver can process up to a certain amount of alcohol before its cells start deteriorating, and its capacity to regenerate tissue diminishes, leading to scarring and loss of functionality. Alcoholic hepatitis is the inflammation of the liver caused by drinking alcohol. It’s most common in people who’ve been alcoholics for multiple years and can lead to death if not treated promptly. Let’s explore everything you should know about alcoholic hepatitis.
Causes and Risk Factors
Like many other illnesses, alcoholic hepatitis results from lifestyle choices, biological and genetic factors, and interactions with other diseases. Of course, one of the most significant culprits behind this disease is alcohol abuse.
Alcoholism or binge drinking
Up to 35% of alcoholics have alcoholic hepatitis. That’s close to five million people in the US alone. Liver damage due to excess and long-term drinking is one of the leading causes of alcoholic hepatitis.
The process of how this damage occurs is unclear, but experts know that the liver tolerates a moderate amount of alcohol. After alcohol consumption regularly exceeds a certain level (which is different for everyone), the liver starts to suffer consequences to its metabolism. At this point, continuing to drink excessive doses of alcohol may lead to fatty liver, the first stage of alcoholic hepatitis.
From there, the illness progresses if the patient doesn’t receive treatment.
Gender
Women are at a higher risk of suffering alcoholic hepatitis than men. Women are generally more vulnerable to the effects of alcohol and alcohol-related organ damage, which makes alcoholic hepatitis more likely to develop in women and more severe.
Age
People of a wide range of ages have alcoholic hepatitis. Still, those between 31 and 55 are more likely to suffer hepatitis, including the alcoholic kind. The typical age for alcoholic hepatitis is between 40 and 50, with most cases recognized before 60.
Genetics
Researchers have identified multiple genes and genetic markers associated with the risk of developing alcoholic hepatitis. Some people are naturally more vulnerable to alcoholic hepatitis due to their genes.
Poor Nutrition
Poor nutrition is common in heavy drinkers because alcohol suppresses hunger. The lack of proper nutrition makes people more vulnerable to liver damage due to the effects of alcohol. High-fat diets are also associated with alcoholic hepatitis.
Other Illnesses And Risk Factors
Multiple medical conditions and lifestyle habits are associated with a higher risk and severity of alcoholic hepatitis, including the following:
- Hepatitis C and other causes of liver damage
- Obesity
- High coffee consumption
- Tobacco use
Symptoms of Alcoholic Hepatitis
Unfortunately, alcoholic hepatitis is challenging to assess. Alcoholic hepatitis can often remain asymptomatic and undiagnosed until the disease progresses into cirrhosis. However, some early signs of hepatitis are essential to recognize.
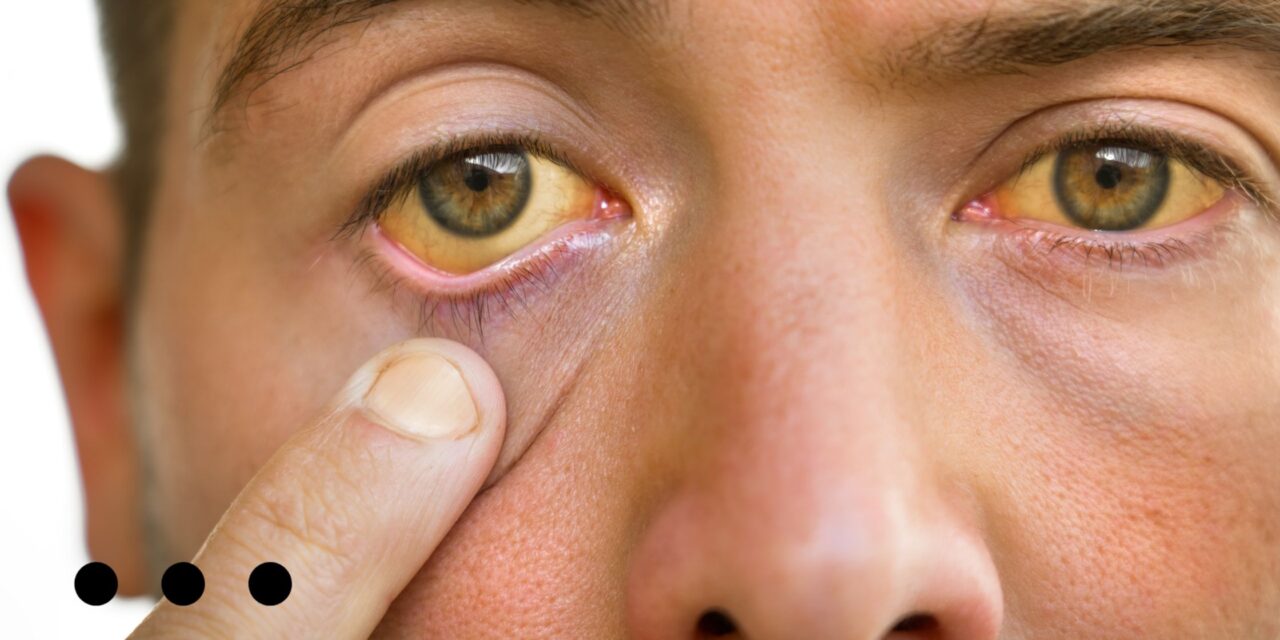
- Jaundice: The yellowing of the skin and the white of the eyes. It’s the most common symptom of alcoholic hepatitis. Jaundice is generally the result of too much bilirubin or the liver’s inability to eliminate it.
- Abdominal swelling and pain: The liver’s inflammation causes pain in and around the area where the liver is.
- Fatigue and weakness: Fatigue and an overall feeling of weakness are common symptoms for multiple types of hepatitis.
- Loss of appetite and weight loss: Loss of appetite is often associated with excessive alcohol consumption, leading to weight loss and malnourishment.
As the illness progresses and liver function degrades, other more severe symptoms appear, such as:
- Fever
- Extreme fatigue and malaise
- Fast and irregular heart rate
- Frequent bruises and bleeding (thrombocytopenia)
- Liver disease-related brain fog, confusion, and cognitive decline (hepatic encephalopathy)
Diagnosis and Treatment
In 2003, about 44% of deaths from liver disease were attributed to alcohol abuse. About 15% of alcoholics in the US eventually developed some sort of alcohol liver disease. Unfortunately, for the most part, alcoholic hepatitis is often misdiagnosed or undiagnosed, which results in underestimated deaths from this condition.
Diagnosis for Alcoholic Hepatitis
The most common evaluations used to diagnose alcoholic hepatitis are:
- Complete blood counts (CBC). A series of blood cell tests to rule out infection, cirrhosis complications, thrombocytopenia, and other symptoms.
- Liver function tests (LFTs)
- Abdominal imaging (abdominal ultrasonography) to look for liver tumors and biliary obstructions.
- Prothrombin time (PT) and INR to assess liver synthetic function
- BMP (basic metabolic profile) to check for renal failure and low potassium and other minerals levels.
- Endoscopy for varices in the esophagus
Early diagnosis is essential to achieve the best outcomes. Unfortunately, most patients with alcohol-related liver diseases are diagnosed at the advanced stages when the symptoms become more severe.
Treatment
Treatment for alcoholic hepatitis depends on various factors, but for the most part, it encompasses a combination of these three approaches:
- Abstinence. Alcohol abstinence is the best way to treat alcoholic hepatitis. Long-term alcohol abuse leads to deteriorating liver tissues and scarring, which can ultimately lead to cirrhosis, the final and most severe stage. Abstaining from alcohol prevents further liver damage and may lead to the regeneration of damaged tissue in less severe cases.
- Nutritional changes. Malnutrition is widespread in alcoholic hepatitis patients. Protein and caloric deficiencies are associated with higher short and long-term mortality rates in patients with acute (severe) alcoholic hepatitis.
- Medication. Doctors may sometimes prescribe anti-inflammatory medication for short-term benefits in severe cases. Corticosteroids are the most common medication prescribed for this, followed by pentoxifylline in patients that suffer significant side effects from corticosteroids.
Prevention And Recovery
People are at different risks of developing alcoholic hepatitis due to their individual, environmental, social, and genetic circumstances. As a result, everyone’s prevention and treatment plan is different.
However, the following strategies are proven effective at preventing alcoholic hepatitis and helping patients recover:
- Reducing but preferably eliminating alcohol consumption. Alcohol abstinence is the best way to prevent alcohol-related liver disease.
- Prevent hepatitis C. Hepatitis C is a contagious disease caused by a virus. Most often, it’s transmitted through drug paraphernalia like needles.
- Consume a balanced diet and exercise regularly. Caloric, protein, and mineral deficiencies are common in people with alcoholic hepatitis. Getting help from nutritionists will help identify nutritional risk factors.
- Seek help for alcohol abuse. If you drink heavily and have not managed to stop or reduce your intake, be aware of common symptoms and seek medical help as soon as you notice them.
- Practice safe medication intake. Don’t mix alcohol with medications that produce side effects when combined with alcohol.
Whether you struggle with alcohol abuse or not, protecting your liver and overall health is essential. Don’t hesitate to speak with an addiction specialist if you or someone you love is dealing with alcohol abuse. Early intervention and treatment are key to preventing long-lasting diseases like alcoholic hepatitis or cirrhosis.